What would be different?
If families, employers and payers could use accurate effectiveness data to decide where to send patients, the best treatment centers would be rewarded with higher reimbursement rates and more clients.
Every rehab and health insurance company would be focused on determining how they could improve their outcomes. KPIs would be based on what really matters – how many patients recover – and payers would stop kicking people out of treatment after only two or three weeks.
Most importantly, lots more people – sons and daughters, husbands and wives, fathers and mothers – would recover from the debilitating addiction that is destroying their (and their family’s) lives.
Sounds like a pipe dream, doesn’t it? Conquer Addiction is in the process of making this happen.
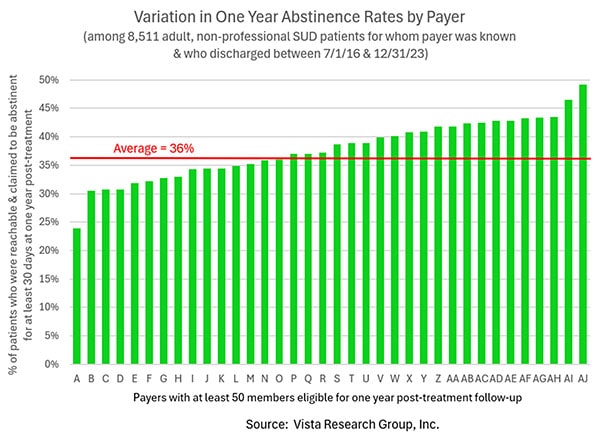
Before we get into the details of what we’re going to do, let’s back up for a minute and talk about the problem. Conquer Addiction’s sister company, Vista Research Group, has monitored over 100,000 patients during addiction treatment and followed up with more than a third of them after treatment. We’ve learned that the one year recovery rates of individuals vary tremendously by both the treatment center they attend and by their health insurance company:
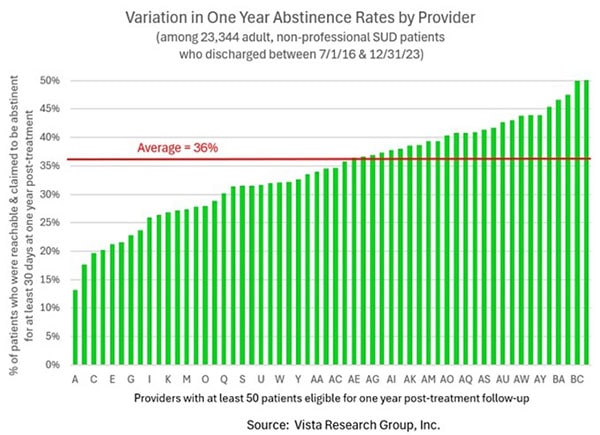
| 
|
Unfortunately, accurate outcomes data exists for only a tiny fraction (well under 1%) of the patients who attend treatment each year.
We need to develop a second source of truth.
Fortunately, one is available. Individuals in the throes of addiction typically have a high number of expensive medical interventions, including emergency room visits, unplanned hospital stays, and detox treatments. Among those patients who are in recovery one year after treatment, there’s a dramatic reduction between the pre-treatment year and the post-treatment year in the number of expensive medical interventions they used:
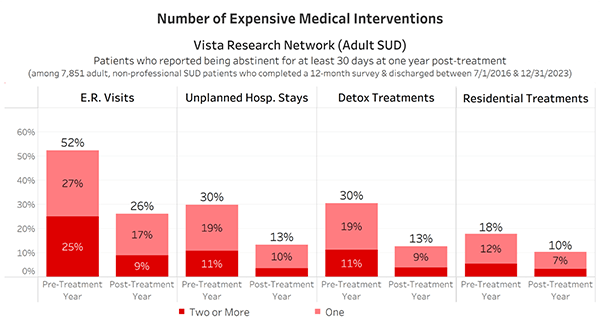
This indicates that claims and death registry data can likely be used to estimate the percentage of patients who achieve recovery following an episode of treatment.
Using Claims & Death Data To Estimate Effectiveness
Conquer Addiction has partnered with companies that have claims data for the majority of Americans and a comprehensive death registry. Because the leaders of these companies want to help many more people recover from addiction, they've agreed to provide their data to Conquer Addiction at substantially discounted rates. Through the magic of tokenization, we can connect health data from multiple sources in a de-identified fashion.
Then we’ll do two things. First, we will create a predictive model that translates claims data into indicators of addictive substance use, and then we will apply it to the data for the majority of patients who attended treatment in a given year.
Creating a Predictive Model: Through our partnerships with other companies, we have access to claims data for 91.5% of the 23,000 SUD patients for whom Vista has one year post-treatment outcomes data on. We will create a matched dataset of claims, outcomes and death registry data and use this one-of-a-kind resource to identify the factors in claims data that predict the likelihood an individual is in recovery one year after treatment.
For example, a patient who is seen in the E.R. for a drug overdose 10 months after treatment is likely to still be using two months later. By comparison, the long-term use of Vivitrol or Suboxone or regular visits to a primary care doctor may be indicators that the individual is doing well. And, of course, a former patient's untimely death is likely to have been caused by a return to use.
Identifying Effective Providers & Payers at Scale: Once the predictive model has been developed, we plan to apply it to claims data for a million or more Americans who attended addiction treatment in 2023. We will use the predictive model to estimate the likelihood that each particular individual is in recovery one year after addiction treatment, then consolidate these predictions for all patients who attended a particular addiction treatment center or were members of a specific health insurance company.
Doing so will give us a data-based method for identifying the most effective addiction treatment providers across the country as well as the health insurance companies funding a sufficient amount of treatment at effective centers. We plan to update these analyses annually.
Bringing Transparency & Accountability to Addiction Treatment
Once we've been able to identify the providers and payers with the best outcomes, it's important to share these findings publicly. We're not into shaming, however, so we'll share their results with each company confidentially and allow them to choose whether or not their results are publicized.
Helping Families Find Effective Treatment Providers: Treatment centers which are proud of their estimated success rates will be invited to publicize their results for a nominal fee (currently $199/year) on Conquer Addiction’s nonprofit website. Treatment centers that choose not to publicize their results will not be identified in any way.
Treatment providers with estimated success rates above 40% based on either outcomes research or claims analysis will be invited to join the Five Star Addiction Treatment Market for the following year. By defining one or more episodes of treatment for an all-inclusive cash price and promising to cover the treatment cost of a second episode of treatment for any patients who relapse within 90 days of completing their program, Market members align their interests with their patients and show how confident they are in their center's effectiveness.
Holding Health Insurers Accountable for Their Outcomes: As shown above, the likelihood an individual is doing well one year post-treatment varies almost as much by health insurance company as it does by the treatment center they attended. Just as it is important for providers to be held accountable for their outcomes, it is crucial that insurers funding only short treatment stays or building networks of less effective centers also be held accountable for their outcomes.
Conquer Addiction will notify payers of the percentage of their patients who are estimated to be in recovery one year post-treatment and offer to publicize their results. Since insurers are anxious to find ways to differentiate themselves to employers, we anticipate that at least some of the insurers with the best outcomes will choose to promote their results publicly. Since “what gets measured gets managed”, we hope this will help galvanize the entire health insurance industry to focus on improving the recovery rate of its members.
How You Can Become Involved
We've set some truly bold and ambitious goals for the Conquer Addiction Moonshot. If you share our dream of helping many more people recover from addiction, please join with us and prove Margaret Mead right:
"Never doubt that a small group of thoughtful, committed citizens can change the world; indeed, it's the only thing that ever has."
We are creating a Moonshot Advisory Board with providers, payers, funders, researchers and patient representatives to help us think through the important questions related to this project. If you’re interested in being involved in this advisory group, please reach out to Joanna Conti at Jconti@vista-research-group.com with a short summary of your qualifications. Our first advisory board meeting will be in April. Thank you!